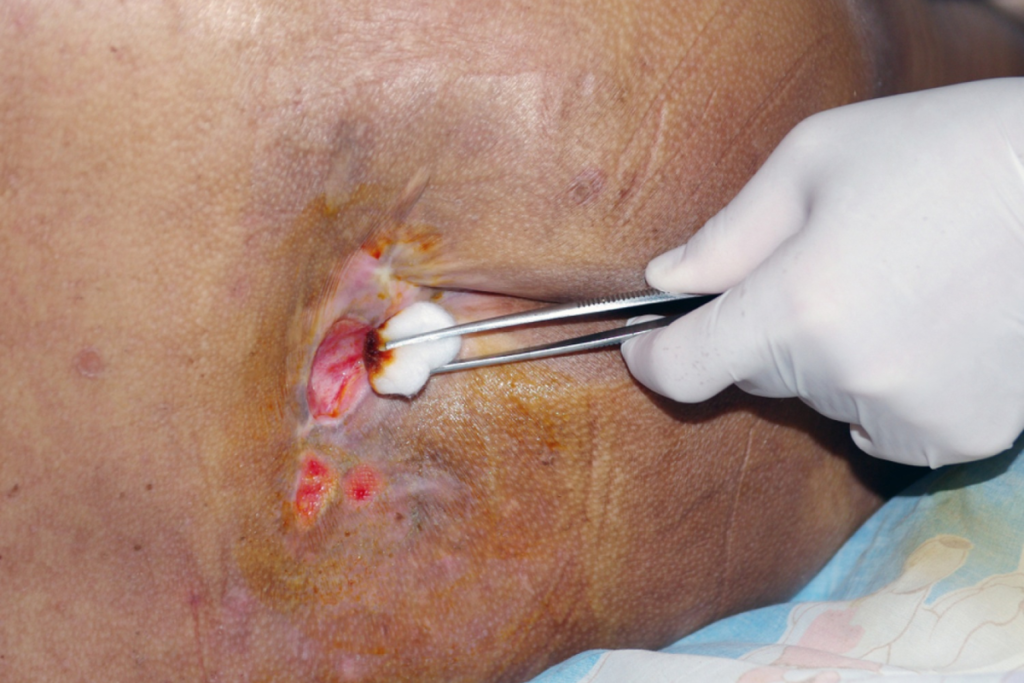
How Decubitus Ulcers Affect the Body
Decubitus ulcers, also known as pressure sores, occur when constant pressure restricts blood flow to specific areas of the body. This reduced circulation deprives tissues of oxygen and nutrients, eventually causing damage. These ulcers most commonly develop in areas where bones press against the skin, such as the lower back, hips, heels, and shoulders. Individuals who spend long periods in one position, especially those who are bedridden or use wheelchairs, face a higher risk. The condition often begins with subtle skin changes that can easily be overlooked. Without timely care, these changes can evolve into deep wounds that are difficult to treat. Decubitus ulcer treatment becomes more intensive as the damage progresses, making awareness and early action essential.
Common Triggers and Underlying Causes
The development of pressure ulcers is influenced by several physical and health-related factors. Prolonged pressure remains the leading cause, as it limits blood flow to the skin. Friction from repeated rubbing against bedding or clothing can weaken the skin’s surface. Shear forces, which occur when the skin moves while underlying tissue remains stationary, further increase the risk. Moisture from sweat or bodily fluids can soften the skin, making it more prone to breakdown. Chronic illnesses such as diabetes and cardiovascular conditions can impair healing and increase vulnerability. Aging skin, which is thinner and less elastic, is also more susceptible to damage. Identifying these triggers is key to implementing effective decubitus ulcer treatment and prevention strategies.
Understanding the Severity Through Staging
Decubitus ulcers are categorized into stages that reflect the extent of tissue damage. Stage 1 involves intact skin with noticeable redness or discoloration that does not fade under pressure. Stage 2 is characterized by partial skin loss, often appearing as a blister or shallow open wound. Stage 3 extends deeper into the tissue, exposing fat and forming a more serious ulcer. Stage 4 represents severe damage where muscle, bone, or tendons may be visible. Some wounds are unstageable due to the presence of dead tissue covering the area. Deep tissue injuries may also occur beneath intact skin, making them harder to detect. Proper staging is essential for determining the most appropriate decubitus ulcer treatment plan and ensuring effective care.
Warning Signs That Indicate Immediate Attention
Recognizing early symptoms of pressure ulcers can prevent the condition from worsening. Persistent redness or unusual discoloration is often the first visible sign. The affected area may feel warmer or cooler than surrounding skin, indicating circulation changes. Patients may experience discomfort, itching, or pain in the area. As the condition progresses, swelling and changes in texture may become apparent. Open sores, blisters, or drainage signal more advanced stages that require prompt intervention. Individuals with limited sensation may not notice these symptoms, making regular skin checks essential. Early identification allows for quicker and more effective decubitus ulcer treatment.
Key Approaches to Decubitus Ulcer Treatment
Treating pressure ulcers effectively requires a combination of strategies that address both the wound and its underlying causes. Relieving pressure is the most critical step, as it allows blood flow to return to the affected area. Proper wound care, including cleaning and dressing, helps prevent infection and supports healing. Maintaining a moist environment encourages tissue regeneration and reduces scarring. Managing underlying health conditions is equally important for successful recovery. Pain management improves comfort and helps patients tolerate necessary treatments. Consistent monitoring ensures that any changes in the wound are addressed promptly. These approaches form the foundation of successful decubitus ulcer treatment.
Modern Medical Treatments and Therapies
Healthcare providers use a variety of medical techniques to treat pressure ulcers based on their severity. Wound cleaning is essential to remove debris and reduce the risk of infection. Specialized dressings are selected to maintain the right balance of moisture and protection. Debridement is often necessary to remove dead tissue and promote healing. This process can be performed surgically, chemically, or through natural methods supported by dressings. Antibiotics may be prescribed when infection is present or likely. Advanced treatments such as negative pressure wound therapy help improve blood flow and accelerate healing. Hyperbaric oxygen therapy may also be used in certain cases to enhance tissue repair. These medical interventions strengthen the effectiveness of decubitus ulcer treatment.
Surgical Solutions for Advanced Pressure Ulcers
In severe cases where other treatments are not effective, surgical intervention may be required. Procedures such as skin grafts and flap reconstruction are used to repair extensive tissue damage. These methods involve transferring healthy tissue to cover the wound and support healing. Surgery can significantly improve outcomes but requires careful preparation and follow-up care. Patients must continue pressure relief measures to prevent recurrence. Recovery involves monitoring for infection and ensuring proper wound healing. Collaboration between surgeons and other healthcare professionals is essential for success. Surgical options provide an important pathway in advanced decubitus ulcer treatment.
The Role of Nutrition in Recovery
Nutrition is a vital component of the healing process for pressure ulcers. Protein is necessary for tissue repair and the formation of new skin cells. Vitamins such as vitamin C play a key role in collagen production and immune support. Minerals like zinc and iron contribute to overall healing and energy levels. Adequate hydration helps maintain skin elasticity and supports bodily functions. Patients with poor nutrition may experience slower recovery and increased risk of complications. A balanced diet tailored to individual needs can significantly enhance healing. Incorporating proper nutrition into decubitus ulcer treatment ensures better outcomes and improved health.
Preventing Pressure Ulcers Before They Start
Preventive care is essential for reducing the risk of developing pressure ulcers, especially in high-risk individuals. Regular repositioning helps relieve pressure and improve circulation. Supportive surfaces, such as specialized mattresses and cushions, distribute weight more evenly. Maintaining good hygiene keeps the skin clean and reduces irritation. Daily skin inspections allow for early detection of potential problems. Encouraging movement, even in limited forms, supports overall health. Educating caregivers and patients about preventive measures ensures consistent care. Prevention is a key element of effective decubitus ulcer treatment and long-term management.
Essential Prevention Habits
- Reposition the body every two hours to reduce pressure
- Use pressure-relieving devices such as cushions and mattresses
- Keep skin clean, dry, and properly moisturized
- Check the skin daily for early signs of damage
- Maintain a diet rich in protein and essential nutrients
- Encourage safe physical activity whenever possible
- Seek medical advice at the first sign of skin breakdown
Providing Effective Care at Home
Home care plays a significant role in managing pressure ulcers, especially for patients who are not hospitalized. Caregivers must follow proper wound care procedures to prevent infection and promote healing. Cleaning and dressing the wound should be done with care and consistency. Using appropriate equipment can improve both patient comfort and treatment effectiveness. Emotional support is also important, as patients may feel discouraged during recovery. Caregivers should monitor for signs of worsening conditions and seek medical help when necessary. Regular communication with healthcare providers ensures that the treatment plan remains effective. With proper guidance, home-based decubitus ulcer treatment can lead to successful recovery.
Risks Associated with Delayed or Inadequate Treatment
Failing to treat pressure ulcers properly can lead to serious complications. Infections may spread to deeper tissues, including bones, resulting in conditions such as osteomyelitis. Severe infections can enter the bloodstream and cause life-threatening conditions like sepsis. Chronic wounds may develop, making healing more difficult and prolonged. Pain and discomfort can significantly affect a patient’s quality of life. Increased healthcare costs and longer recovery times are also common. Early and consistent decubitus ulcer treatment is essential to avoid these risks. Addressing the condition promptly ensures better outcomes and improved well-being.
Collaborative Care for Better Results
Managing pressure ulcers often requires a team of healthcare professionals working together. Doctors oversee diagnosis and treatment plans, ensuring that care is tailored to the patient’s needs. Nurses handle wound care and monitor progress regularly. Physical therapists help improve mobility and reduce pressure on vulnerable areas. Nutritionists provide dietary guidance to support healing. This collaborative approach ensures that all aspects of care are addressed. Each team member contributes expertise that enhances the effectiveness of decubitus ulcer treatment. Team-based care leads to improved healing outcomes and patient satisfaction.
Innovations Improving Pressure Ulcer Management
Advancements in medical technology are transforming how pressure ulcers are treated. Smart dressings can monitor wound conditions and provide valuable data for healthcare providers. Regenerative medicine offers new possibilities for repairing damaged tissue. Telemedicine allows for remote monitoring and consultation, improving access to care. These innovations make treatment more efficient and personalized. Patients benefit from faster healing and improved comfort. Ongoing research continues to explore new methods for enhancing outcomes. Staying informed about these developments helps patients and caregivers make better decisions regarding decubitus ulcer treatment.
Frequently Asked Questions
What is the best way to treat a decubitus ulcer
The best approach involves relieving pressure, maintaining proper wound care, and addressing underlying health conditions.
Can pressure ulcers heal completely
Yes, with proper care and early treatment, many pressure ulcers can heal fully.
How long does it take for a pressure sore to heal
Healing time varies depending on severity and overall health, ranging from weeks to months.
Are pressure ulcers preventable
Yes, most pressure ulcers can be prevented with proper care, repositioning, and hygiene.
Is professional medical care always necessary
Mild cases may be managed at home, but moderate to severe ulcers require medical attention.
What should caregivers focus on most
Caregivers should focus on pressure relief, wound care, nutrition, and monitoring for signs of infection.
Takeaway
Decubitus ulcer treatment requires consistent care, early detection, and a comprehensive approach that addresses both healing and prevention. By understanding the causes, recognizing warning signs, and applying proper treatment methods, patients and caregivers can significantly improve recovery outcomes. Support from healthcare professionals, combined with proper nutrition and daily care practices, plays a crucial role in restoring skin health and preventing future complications.