Clinical Scope of Sever Wound Surgery in Modern Trauma Systems
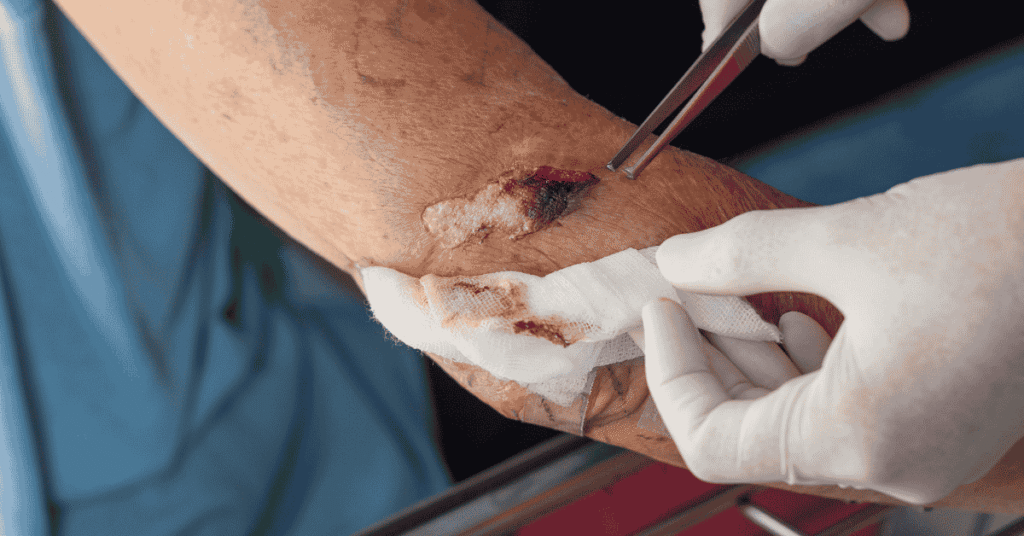
Sever wound surgery refers to a set of emergency surgical procedures designed to treat life-threatening injuries involving extensive damage to skin, muscle, bone, nerves, and blood vessels. It is a core component of trauma medicine and is typically performed when conventional wound care cannot stabilize the injury or prevent rapid deterioration. This form of surgery is commonly carried out in emergency departments, trauma centers, and specialized surgical units equipped for high-acuity cases. The procedure requires immediate collaboration among multiple surgical specialties to ensure that all aspects of the injury are addressed effectively. In many cases, sever wound surgery is performed under extreme time pressure, where rapid clinical judgment directly impacts patient survival. The primary objective is to control bleeding, prevent infection, and restore structural integrity as quickly as possible. Because of the complexity of injuries involved, sever wound surgery is considered one of the most demanding areas of emergency surgical care.
Types of Traumatic Injuries Requiring Sever Wound Surgery
Sever wound surgery is required for a wide range of traumatic injuries that compromise the body’s structural and functional systems. Deep lacerations are among the most common, often involving multiple layers of tissue and heavy bleeding. Crush injuries occur when significant force compresses body parts, leading to tissue destruction and vascular compromise. Avulsion injuries involve the tearing away of skin or soft tissue, frequently requiring reconstructive grafting. Penetrating trauma, such as stab wounds or projectile injuries, can damage internal organs and blood vessels. Degloving injuries are particularly severe and involve the separation of skin from underlying structures over large areas. Open fractures often accompany severe soft tissue damage and significantly increase infection risk. Each of these injury types requires a tailored surgical approach to ensure effective treatment and recovery.
Common Causes Behind Severe Wounds Requiring Surgical Intervention
Severe injuries requiring sever wound surgery often result from high-energy traumatic events. Road traffic accidents are a leading cause, particularly those involving high-speed impacts or pedestrian collisions. Workplace accidents involving heavy machinery or industrial tools frequently produce complex wound patterns. Falls from significant heights can result in combined fractures and deep tissue injuries requiring immediate surgical repair. Sports-related trauma, especially in contact or extreme sports, can lead to severe musculoskeletal damage. Explosions and blast injuries introduce additional complications due to pressure waves and foreign debris embedded in tissue. Animal attacks may cause deep puncture wounds and tearing injuries requiring surgical intervention. Burns and chemical exposure can also destroy skin and underlying tissues, making reconstructive surgery essential.
Emergency Stabilization Prior to Sever Wound Surgery
Before sever wound surgery is performed, emergency stabilization is critical to preserve life and prevent further injury. Airway management ensures that the patient maintains adequate oxygen supply during critical moments. Breathing and circulation support are prioritized to prevent shock and organ failure. Severe bleeding must be controlled immediately using pressure dressings, tourniquets, or surgical clamps. Temporary wound coverings are applied to reduce contamination and protect exposed tissues. Pain management is carefully administered to avoid destabilizing the patient’s condition. Emergency teams also assess injury severity to determine transport urgency to surgical facilities. Communication between field responders and hospital teams ensures readiness for immediate surgical intervention upon arrival.
Diagnostic Evaluation in Sever Wound Surgery Cases
Accurate diagnosis is essential for planning effective sever wound surgery. Physical examination provides initial insight into wound depth, bleeding severity, and tissue damage. X-rays are used to detect fractures and bone misalignment. CT scans offer detailed imaging of internal injuries, including organ and vascular damage. Ultrasound imaging helps assess blood flow and identify hidden injuries. Laboratory tests evaluate infection risk, blood loss, and overall physiological stability. Neurological assessments are performed when nerve or spinal injuries are suspected. These diagnostic tools collectively guide surgical decision-making and determine the urgency and scope of intervention.
Surgical Planning and Preparation for Sever Wound Surgery
Surgical planning is a structured process that ensures safe and effective sever wound surgery. Stabilization of vital signs is the first priority before any operative procedure begins. Surgeons evaluate the extent of injury and anticipate possible complications. The choice of surgical technique depends on the type and severity of the wound. Anesthesia planning ensures that the patient remains stable and pain-free throughout the procedure. Multidisciplinary coordination is often required for complex trauma cases involving multiple body systems. Surgical instruments and sterile environments are prepared in advance to reduce infection risk. Even in emergency situations, careful planning improves surgical outcomes significantly.
Core Surgical Procedures in Sever Wound Surgery
Sever wound surgery involves multiple essential procedures aimed at restoring tissue integrity and preventing complications. Debridement is performed to remove dead or contaminated tissue that could lead to infection. Hemostasis techniques are used to control bleeding and stabilize blood vessels. Muscle and soft tissue repair helps restore structural function and support. Bone realignment and fixation are required when fractures are present. Skin closure may involve sutures, staples, or surgical adhesives depending on wound severity. Temporary closure techniques may be used in cases requiring staged reconstruction. These procedures form the foundation of emergency trauma surgical care.
Reconstructive Surgery After Sever Wound Procedures
Reconstructive techniques are vital for restoring function and appearance after sever wound surgery. Microsurgery enables precise repair of small blood vessels and nerves. Skin grafting replaces lost tissue using donor skin from other body areas. Tissue expansion techniques allow for gradual growth of healthy skin for reconstruction. Flap surgery transfers tissue to cover large or complex wounds. Biomaterials are sometimes used to support healing and tissue regeneration. Advances in regenerative medicine continue to improve reconstruction outcomes. These methods play a crucial role in long-term recovery and functional restoration.
Infection Control and Postoperative Wound Care
Infection control is a critical component of recovery following sever wound surgery. Antibiotic therapy is commonly used to prevent or treat bacterial infections. Regular dressing changes maintain a sterile environment around the wound. Medical teams monitor for signs of infection such as swelling, fever, or discharge. Severe infections may require additional surgical intervention to remove infected tissue. Drainage systems help prevent fluid accumulation in surgical sites. Negative pressure wound therapy promotes healing by improving circulation. Proper postoperative care significantly reduces complication risks and enhances recovery.
Pain Management and Recovery Support Systems
Pain management is essential after sever wound surgery to ensure patient comfort and recovery progress. Medication plans are customized based on injury severity and patient response. Non-opioid pain relievers are often used to minimize dependency risks. Physical therapy is gradually introduced to restore movement and strength. Psychological support helps patients manage emotional trauma associated with severe injuries. Nutritional support enhances tissue repair and immune system function. Sleep regulation contributes to faster healing and recovery stability. Comprehensive support systems improve both physical and mental recovery outcomes.
Complications Associated With Sever Wound Surgery
Complications may occur despite advanced surgical techniques in sever wound surgery. Delayed wound healing can result from infection or poor circulation. Excessive scar formation may affect mobility and appearance. Nerve damage can lead to loss of sensation or motor function. Secondary infections remain a serious concern during recovery. Blood clots may form and require medical intervention. Graft failure can occur if transplanted tissue does not integrate properly. Chronic pain may persist long after initial healing has occurred.
Rehabilitation and Long-Term Recovery Process
Rehabilitation is essential for restoring function after sever wound surgery. Physical therapy helps rebuild strength, flexibility, and coordination. Occupational therapy focuses on restoring daily living skills and independence. Assistive devices may be used during early recovery stages. Long-term follow-up ensures proper healing and functional progress. Additional reconstructive procedures may be required in some cases. Lifestyle adjustments support sustained recovery and health improvement. Emotional rehabilitation is also important for psychological stability and adjustment.
Prevention Strategies for Reducing Sever Wound Surgery Cases
Preventing injuries that require sever wound surgery involves multiple safety measures. Workplace safety programs reduce the risk of industrial accidents. Road safety awareness helps prevent traffic-related trauma. Protective equipment in sports minimizes injury severity. Fire safety practices reduce burn-related injuries. Public education increases awareness of injury prevention strategies. Emergency preparedness training improves response effectiveness during accidents. Early intervention reduces injury severity and improves survival rates.
Technological Innovations in Sever Wound Surgery
Modern technology has significantly improved sever wound surgery outcomes. Robotic-assisted surgery enhances precision and reduces human error. 3D printing allows for customized implants and reconstructive models. Advanced imaging improves diagnostic accuracy and surgical planning. Bioprinting research explores tissue regeneration possibilities. Smart wound dressings monitor healing progress in real time. Artificial intelligence supports trauma assessment and decision-making. Minimally invasive techniques reduce recovery time and surgical complications.
Ethical Considerations in Emergency Trauma Surgery
Ethical decision-making is a key part of sever wound surgery practice. Medical teams must prioritize patients based on injury severity and survival likelihood. Emergency conditions often require rapid decisions under pressure. Consent challenges arise when patients are unconscious or unable to communicate. Resource allocation becomes critical in mass casualty situations. Cultural and personal beliefs may influence treatment decisions. Proper documentation ensures accountability and transparency. Ethical frameworks guide responsible medical practice in trauma care.
Frequently Asked Questions (FAQ)
What is sever wound surgery used for?
Sever wound surgery is used to treat severe traumatic injuries involving deep tissue damage, heavy bleeding, and structural disruption that cannot heal without surgical intervention.
How urgent is sever wound surgery?
It is highly urgent and is typically performed as soon as the patient is stabilized to prevent complications or death.
Who performs sever wound surgery?
It is performed by trauma surgeons, often supported by orthopedic, vascular, and reconstructive specialists.
What are the risks involved?
Risks include infection, delayed healing, scarring, blood clots, and possible loss of function depending on injury severity.
How long does recovery take?
Recovery may take several weeks to months depending on the severity of the injury and rehabilitation progress.
Can patients fully recover?
Many patients regain significant function, but outcomes depend on injury complexity and treatment quality.
Is rehabilitation necessary?
Yes, rehabilitation is essential for restoring movement, strength, and daily function.
Takeaway
Sever wound surgery is a critical component of trauma medicine designed to save lives and restore function after severe injuries. Its success depends on rapid emergency response, precise surgical intervention, advanced reconstruction techniques, and structured rehabilitation. Ongoing medical advancements continue to improve outcomes, but recovery remains closely tied to coordinated care and long-term patient commitment.